General anesthesia
Table of Contents
Anesthesia meaning
General anesthesia are agent that bring about reversible loss of sensation and consciousness. Before 1846, alcohol, opium, packing limb with ice and concussion, i.e. making the patient unconscious by a blow on head were used to relieve surgical pain. Dr Horace Wells a dentist, tried to demonstrate effect of nitrous oxide as an anesthetic in 1844 but was unsuccessful as he removed the gas bag too early. Dr William Morton who was present at the demonstration, worked on it and in 1846 demonstrate either anesthesia successfully. Since then several anesthesia have been synthesized over the decades.
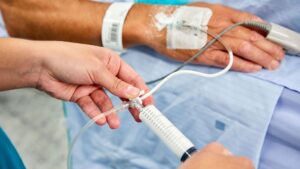
Ideal General anesthesia
- Pleasant
- Nonirritating
- Adequate analgesia
- Immobility
- Muscle relaxation
- Non inflammable
- Administration should be easy
- Wide margin of safety
- It should not affect cardiovascular functions.
- It should be inexpensive.
Types of General anesthesia
Inhalational
- A. Gases – Nitrous oxide, cyclopropane
- B . Liquids – Ether, halothane, enflurane, isoflurane, methoxyflurane
Intravenous
- A. Inducing agents – Thiopentone sodium, methohexitone, propofol, etomidate
- B. Dissociative anesthesia – Ketamine
- Neuro-leptanalgesia – Fentanyl + Droperidol
- Benzodiazepines – Diazepam, lorazepam,
midazolam
INHALATIONAL ANESTHESIA
Nitrous oxide
Nitrous oxide is gas with a slightly sweetish odor. It produces light anesthesia without the significant depression of respiration or vasomotor center.
Advantages of nitrous oxide
- Strong analgesic.
- Induction is rapid and smooth.
- It is non-irritating and non-inflammable
- Recovery is rapid.
- Postoperative nausea is not significant.
- Has little effects on respiration and cardiovascular functions, hence ideal for combination.
Disadvantages of nitrous oxide
- It is less potent and should be used with other
agents - Poor muscle relaxant.
- It is less potent and should be used with other
Ether
Ether is a colorless volatile liquid. It’s highly inflammable; vapors are irritating.
Advantages of Ether
- Potent and reliable anesthetic
- Good analgesic.
- Effects on cardiovascular and respiratory functions are not significant; reflexes are
well-maintained. - It is a bronchodilator
- Provides full muscle relaxation in deep anesthesia.
- Inexpensive
Disadvantages of Ether
- Induction is slow and unpleasant
- It is inflammable—hence diathermy is
contraindicated. - It is irritating and therefore enhances respiratory secretions.
- Postoperative nausea and vomiting are frequent.
- Recovery is slow
Halothane
Halothane is a colorless volatile liquid with a sweet odor. It is non-irritant and non-inflammable.
Advantages of Halothane
- Potent, non-inflammable anesthetic
- Induction is smooth and rapid—in 2-5 minutes anesthesia can be produced.
- Non-irritant—therefore does not increase salivary or bronchial secretion.
- Recovery is rapid.
- Postoperative nausea and vomiting is of low
incidence.
Disadvantages of Halothane
- Halothane is a direct cardiac depressant. Cardiac output and BP start falling and heart
rate may decrease. It sensitizes the heart to actions of adrenaline. - Not a good analgesic; not a muscle relaxant.
- It also causes some respiratory depression.
- Severe hepatitis which may be fatal occurs rarely
- Expensive
- Halothane is a direct cardiac depressant. Cardiac output and BP start falling and heart
Desflurane and sevoflurane
Desflurane is pungent—may induce coughing and sometimes laryngospasm.
Sevoflurane is chemically unstable. A metabolite of sevoflurane may cause renal damage. If these disadvantages of sevoflurane could be overcome, we may have found ideal anesthetic.
INTRAVENOUS ANESTHESIA
Intravenous anesthesia allow an extremely rapid induction because the blood concentration can be raised rapidly—in one arm-brain circulation (~ 11 sec) there is loss of consciousness. These are used for induction because of rapid onset of action and anesthesia is maintained by inhalational agent.
INDUCING AGENTS
Thiopentone sodium
Thiopentone sodium is an ultrashort-acting barbiturate which when administered IV. On IV injection it produces unconsciousness in 20-30 sec. It is highly lipid soluble; duration of action is 4-7 minutes. It gets rapidly redistributed in the body tissues
Advantages of Thiopentone sodium
- Quick onset of action; induction is
smooth, rapid and pleasant.
- Quick onset of action; induction is
Disadvantages of Thiopentone sodium
- Not a good anesthesia nor muscle relaxant. Thiopentone sodium cannot be used alone as the dose required results in respiratory and circulatory depression.
Adverse effects
- Respiratory depression,
- Hypotension
- Hiccoughs
Propofol
Propofol is oily liquid; quick induction (30 sec) and recovery (4 min) is possible from single dose. It is used for induction and maintenance for short procedures of up to 1 hour duration.
DISSOCIATIVE ANESTHESIA
Ketamine
Ketamine hydrochloride given 1-2 mg/kg slow IV or 10 mg/kg IM produce dissociative anesthesia within 3-5 min which last for 10-15 min after single injection . Amnesia lasts for 1-2 hr. Premedication with atropine is needed. Return to consciousness is gradual
Advantage of Ketamine
- Provides profound analgesia and can be used as a single agent for minor procedures.
- Respiration is not depressed, does not induce hypotension.
- Less likely to induce vomiting.
- Pharyngeal and laryngeal reflexes are only slightly affected
- It’s particularly useful in children and poor risk patients and also in asthmatic patients since it does not induce bronchospasm.
Disadvantages of Ketamine
- Hallucination and involuntary movement may occur during recovery.
- May be dangerous in hypertensives as it raises the BP.
NEUROLEPTANALGESIA
A combination of fentanyl and droperidol is used.
Droperidol
Droperidol is a rapidly acting, potent neuroleptic
related to haloperidol.
When combination is given IV, a state of neuroleptanalgesia’ is produced. This is characterized by calmness, psychic indifference and intense analgesia without loss of consciousness. It lasts for 30-40 min. Fentanyl 0.05 mg + droperidol 2.5 mg/ml—4 to 6 ml is infused IV over 10 min.
During recovery extrapyramidal symptoms may be seen—due to droperidol. It is employed for endoscopies, burn dressing, angiographies and other diagnostic and minor surgical procedures.
BENZODIAZEPINES
Benzodiazepines like diazepam, lorazepam and midazolam are used to induce or supplement
a. They cause sedation, amnesia and reduce anxiety which are beneficial in such
patients. BZD may be employed alone in procedures like endoscopies, reduction of fractures cardiac catheterization and cardioversion. IV midazolam is particularly preferred as it is faster and shorter-acting, more potent and does not cause pain or irritation at the injection site. BZDs are
also used as preanesthetic medication.
PREANESTHETIC MEDICATION
Prior to anesthesia, certain drugs are administered
in order to make anesthesia safer and more
pleasant and is known as preanesthetic medication. It is given in order to:
- Decrease anxiety.
- Provide amnesia for the preoperative period.
- Relieve preoperative pain if present.
- Make anesthesia safer.
- Reduce side effects of anesthetics.
- Reduce gastric acidity
Sedative hypnotics:
Diazepam 5-10 mg is given orally. It also produces amnesia. Barbiturates are not preferred due to disadvantages like respiratory depression.
Antihistamines
Antihistamines have sedative, antiemetic and anticholinergic properties and are useful, example:- promethazine.
Antiemetics
Antiemetics: Metoclopramide, domperidone or ondansetron may be used. Antihistamines with antiemetic properties may also be used for this purpose.
Anticholinergic drugs
Some irritant anesthetics like ether increase the salivary and respiratory secretions. The secretions from the oral cavity may enter into the larynx causing various problems including laryngospasm and aspiration pneumonia. Hence we need drugs that reduce these secretions. But we now have less irritant anesthetics and secretions are less of a problem. Atropine, scopolamine or glycopyrrolate can be used.
Drugs that reduce acidity
H2 blockers like ranitidine decrease gastric acid secretion and are given on the night before surgery. Decrease in gastric secretions reduces the damage to lungs if aspiration occurs when the patient is on anesthesia.
Gastrokinetic agents
Metoclopramide is a dopamine antagonist that promotes gastrointestinal motility and increases tone of esophageal end of the stomach. This speeds up gastric emptying. The combination of an H2 blocker + metoclopramide provides best protection against aspiration.
Opioids
Like morphine and pethidine reduce anxiety and apprehension, provide analgesia and reduce dose of the anesthetic required.
Balanced anesthesia
Since it is not possible to achieve ideal anesthesia with a single drug, multiple drugs are employed—preanesthetic medication, IV anesthetics for induction, inhalational agents for maintenance, oxygen, skeletal muscle relaxants and analgesics to attain balanced anesthesia
