Fracture healing
Table of Contents
Bone healing
The fracture healing is in many ways similar to the healing of soft tissue wounds, except that soft tissue heals with fibrous tissue, and end result of fracture healing is mineralized mesenchymal tissue, i.e. bone.
Stages in fracture healing of cortical bone
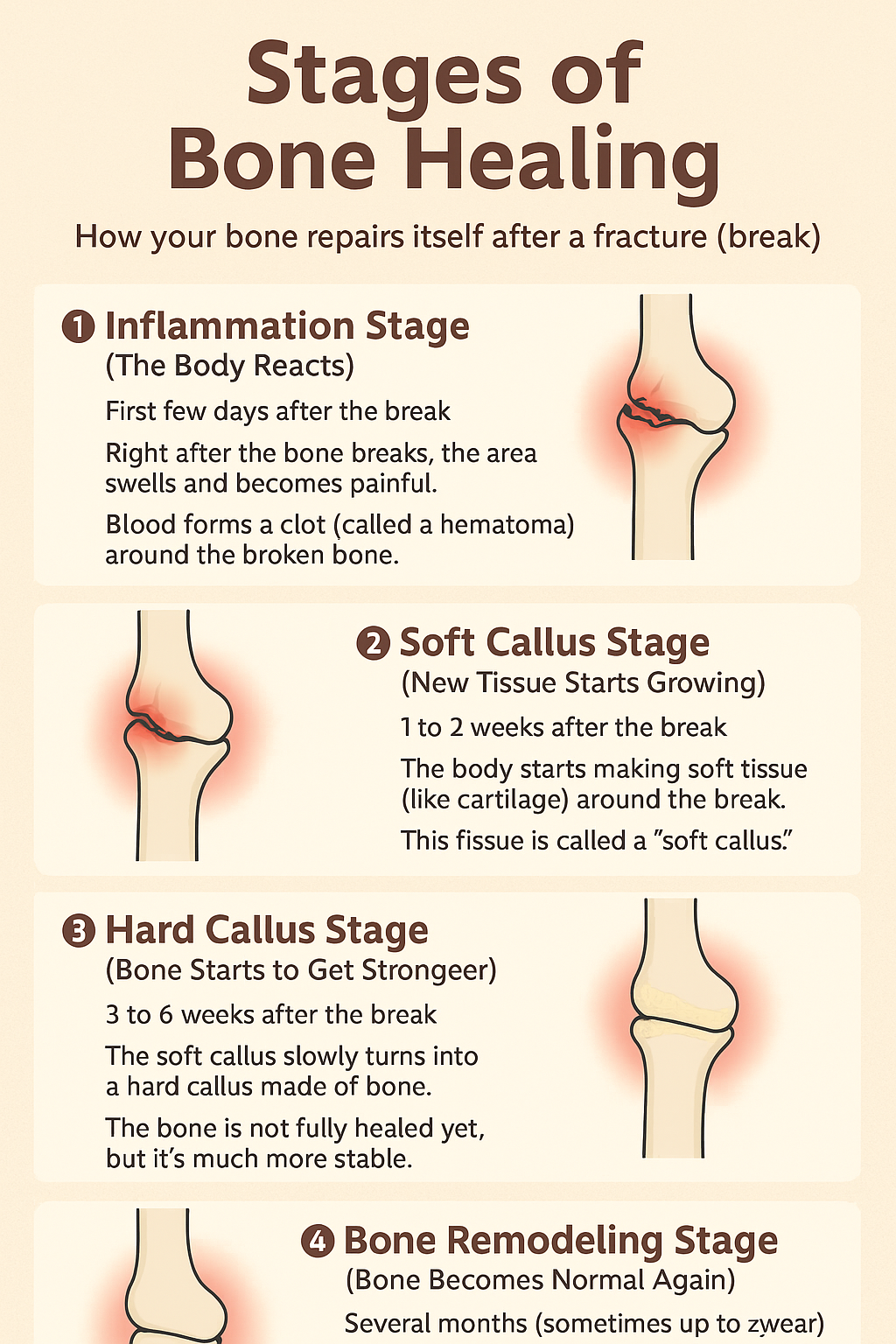
- Stage of hematoma
- Stage of granulation tissue
- Stage of callus
- Stage of remodeling (formerly called consolidation)
- Stage of modelling (formerly called remodeling)
Stage of hematoma
This Stage is also known as the Inflammation Stage (0–7 Days). Just after the bone breaks, the first thing we observed is redness, swelling, and pain, indicating inflammation at that area. When the bone breaks, blood vessels in the area also get damaged, leading to bleeding and the formation of a blood clot (hematoma).T his clot helps stop further bleeding and provides a base for healing. White blood cells and other healing cells rush to the site to clean up the debris and prepare the area for the next stage.
- This stage lasts up to 7 days. When bone is fractured, blood leaks out through
torn vessels in the bone and forms a hematoma between and around the fracture - The periosteum and local soft tissues are stripped from fracture ends
- This results in ischemic necrosis of the fracture ends over a variable length, usually only
a few millimeters.
Stage of granulation tissue
This Stage is also known as the Soft Callus Formation (1–3 Weeks). This typically begins within a few days to a week after the fracture and lasts for approximately 2–3 weeks. This soft callus is composed of cartilage and fibrous tissue, and it holds the bone together; however, it’s still not very strong and can be easily damaged. Avoid putting too much pressure on the bone.
- This stage lasts for about 2-3 weeks. In this stage, sensitized precursor cells (daughter cells) produce cells that differentiate and organize to provide blood vessels, fibroblasts, osteoblasts, etc.
- From this stage, the healing of bone differs from that of soft tissue. In soft tissue healing, the granulation tissue is replaced by fibrous tissue, whereas in bone healing, the granulation tissue further differentiates to create osteoblasts, which subsequently form bone.
Stage of callus
This Stage is also known as the Hard Callus Formation (3–6 Weeks). The transformation of the soft callus into a hard callus. The body starts laying down new bone cells (called osteoblasts), which turn the soft tissue into hard bone. This makes the area much stronger and less painful. X-rays usually show visible healing during this phase.
- This stage lasts for about 4-12 weeks. In this stage, the granulation tissue
differentiates further and creates osteoblasts. - These cells lay down an intercellular matrix, which soon becomes impregnated with the calcium salts.
- Callus formation is slower in adults than in children, and in cortical bones than in cancellous bones.
Stage of remodeling
In this phase, the new bone is gradually reshaped and smoothed to match the bone’s original shape. Excess bone is removed, and the inner bone structure becomes more compact and strong. When the bone returns to its normal appearance and strength. In many cases, the healed bone may become even stronger than before the injury.
- In this stage, the woven bone is replaced by mature bone with a typical lamellar
structure. It is a slow process and takes anything from one to four years. - In this stage, the bone is gradually strengthened. The sharpening of cortices occurs at
the endosteal and periosteal surfaces. The major stimulus to this process comes from local bone strains, i.e., weight-bearing stresses and muscle forces, when a person resumes activity - This stage is more conspicuous in children with an angulated fracture. It occurs to a very limited extent in fractures in adults.
Factors affecting fracture healing
Age of the patient
Fractures unite faster in children. In younger children, callus is often visible on X-rays as early as two weeks after fracture. On average, bones in children unite in half the time compared to those in adults. Failure of the union is uncommon in the fracture of a child.
Pattern of fracture
Flat and cancellous bones unite faster than tubular and cortical bones.
Pattern of fracture:
Spiral fractures unite faster than oblique fractures, which in turn unite faster than transverse fractures. Comminuted fractures usually result from a severe trauma or occur in osteoporotic bones, and thus heal more slowly.
Type of reduction:
Good apposition of the fracture results in faster union. At least half fracture surface should be in contact for optimal union in adults.
Immobilization:
It is not necessary to immobilize all fractures (e.g., fractures ribs, scapula, etc). They heal anyway. Some fractures need strict immobilization (e.g., fracture of the neck of the femur), and may still not heal.
Open fractures:
Open fractures often go into delayed union and non-union.
Compression at the fracture site:
Compression enhances the rate of union in cancellous bone. In cortical bones, compression at the fracture site enhances rigidity of fixation and possibly results in primary bone healing.
Disturbed pathoanatomy
In the former, the fracture ends pierce through the surrounding soft tissues. Since vascularized bone ends are important for optimal fracture union, these fractures unite slowly or do not unite at all.
Healing of cancellous bones
The healing of fractured cancellous bones follows a different pattern. The bone is of uniform spongy texture and has no medullary cavity
Union can occur directly between bony trabeculae.
After haematoma and granulation formation, mature osteoblasts lay down woven bone in the intercellular matrix, and the two fragments unite
Primary and secondary bone healing
Primary fracture healing occurs where the fracture hematoma has been disturbed, as in fractures treated operatively. The bone heals directly, without callus formation, and it is therefore difficult to
Evaluate the union on X-rays.
Secondary fracture healing occurs in fractures where the fracture haematoma is
not disturbed, as in cases treated non-operatively. There is healing, with callus formation, and it can be evaluated on X-rays.
