Osteomyelitis
Table of Contents
Introduction
Infection of the bone by micro-organisms is called osteomyelitis. The microorganism causing infection is a pyogenic organisms(bacteria ) which produce pus in bone. Some common pyogenic organism (bacteria) are Streptococcus, Staphylococcus, Neisseria, and Haemophilus . Bone infection can be acute (recent ) or chronic (long lasting ) .
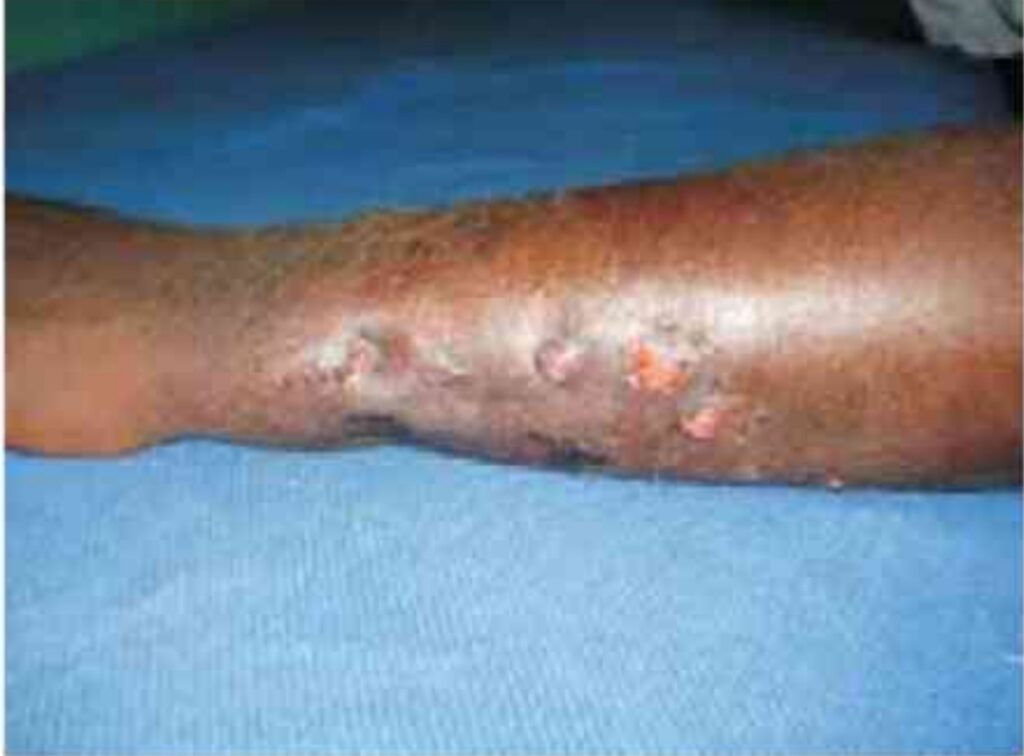
How the microorganisms enter the body?
Microorganisms may enter and infect the bone by any of the following three routes:
Haematogenous route: Most common entry through the bloodstream, common in children (osteomyelitis)
Direct route: Directly through the neighbouring infected tissue (septic arthritis)
Exogenous route: Through open fracture, open wound, surgical incision, etc.
Types of osteomyelitis
Their are three types of osteomyelitis. To know more about bone then see
Acute Haematogenous osteomyelitis
Acute haematogenous osteomyelitis is mostly caused by S. aureus. Streptomyces albus or streptococcus. It occurs most commonly during active growth, i.e., between 3 and 16 years of age. The causative organisms spread through the bloodstream from the original focus such as tonsils, respiratory tract and intestines to the bone.
Clinical features
The onset of Osteomyelitis symptoms may be preceded by a history of trauma to the affected part, in the acute stage presents with high fever, headache, irritability and mild swelling. The diagnosis is important and is done clinically. Some visible osteomyelitis symptoms are,
- A primary focus of infection in the body, e.g., skin and tonsils.
- On examination, signs of dehydration may be found.
- Tenderness and signs of inflammation are present over the metaphysis.
- Swelling may become apparent when the pus comes into a muscular or subcutaneous plane.
- In rare cases, there may be signs of toxaemia.
Investigations
The following investigations may help in osteomyelitis diagnosis, though they may not be specific.
- Blood
(a) Leucocytosis should be up to 20,000 cells.
(b) Erythrocyte sedimentation rate (ESR) level is elevated.
(c) Blood culture may be positive for the organism.
- Radiograph of the affected part
(a) The radiograph is usually normal in the first week.
(b) A periosteal reaction may be seen between 7 and 10 days.
- Bone scan:
It shows an increased uptake by the affected bone.
Treatment
The successful Osteomyelitis Treatment involve its early diagnosis with conservative treatment, surgical treatment and physiotherapy intervention.
Conservative treatment
- Antibiotics: Appropriate antibiotics are administered intravenously.
- Rest and proper positioning of the limb (area of infection) with a suitable POP cast with the limb elevated
- The patient should have an adequate balanced diet and proper fluid intake.
- Regular monitoring of the general condition, fever, pulse and the state of hydration, etc., has to be done.
- Observe edemas, redness of skin, warmth, soft tissue abscess and discharge, etc.
- If the patient is anaemic, then IV fluids are administered in case of dehydration.
Surgical treatment
If there is no response from conservative treatment within 48 hr then surgery is advised. For the incision and drainage of pus from the subcutaneous abscess, multiple holes are drilled into the cortex of the bone for proper drainage of the pus. Sometimes, a small window may be made in the cortex of the bone for better drainage
Exogenous osteomyelitis
Exogenous osteomyelitis is a type in which a microorganism enters through an open wound, an open fracture or following surgery. It can be prevented by early surgical intervention.
Chronic osteomyelitis
Acute osteomyelitis if treated abnormally can lead to chronic osteomyelitis. Another cause can be the weak immunity of the host, it can be due to malnutrition.
Clinical features
- Discharging sinus
- Irregular thickening of the bone
- The irregular surface of the bone
- Deformity of the limb
- Shortening of the limb
- Joint stiffness
Chronic osteomyelitis Treatment
The successful Chronic osteomyelitis treatment involves its early diagnosis with conservative treatment, surgical treatment and physiotherapy intervention.
Antibiotics: Antibiotics are given as per the pus culture and sensitivity reports.
Surgical operations: The following surgical operations are performed either singly or in combination.
Sequestrectomy: Removal of the necrotic bone (sequestrum) with curettage of the cavity is carried out.
Curettage: The cavity in the bone allows accumulation of pus and bacteria inside it. The cavity is curetted and after a thorough curettage, it may be filled with cancellous bone grafts or a viable muscle.
Saucerization: Pus gets collected in the deep cavity of the bone. The cavity is therefore made shallow like a ‘saucer’, by removing its overhanging edges which prevents accumulation of pus. This procedure is called sauterization.
Excision of the sinus tract: The sinus tract is excised and the wound is allowed to heal slowly.
Amputation: It is done in rare cases where organs get affected due to injection.
Subacute osteomyelitis
Subacute osteomyelitis is of three types: Salmonella osteomyelitis, Brodie abscess and Sclerosing osteomyelitis of Garre.
Clinical features
- Chronic dull pain over the site of the lesion (usually tibia) which worsens at night.
- Deep bony tenderness
- No discharging sinus
Treatment
Successful bone infection treatment involves its early diagnosis with conservative treatment, surgical treatment and physiotherapy intervention.
- Antibiotics
- Excision of the thickened bone
- Differentiation from Ewing sarcoma, osteosarcoma, or osteoid osteoma which have a similar radiographic picture.
Physiotherapy Intervention
Initial Stage
Cryotherapy: Pain and muscular spasms should be controlled with ice packs or ice water packs.
Splinting: The affected joint in a functional position should be done.
Elevated position: The affected limb should be comfortably placed in an elevated position to reduce oedema.
Active full range: Unaffected joints are moved through the active full range.
Isometrics: Brief and light isometrics are initiated to the muscles within the pain-free range.
No weight bearing: The mother of the child should be warned not to allow or hastily carry out by the affected limb.
Self-resistive modes of exercise: The unaffected joints are guided and supervised.
Late stage
Rhythmic relaxed self-active movements: Within the pain-free ROM.
Educate mother: Wherever possible, educate the mother to encourage the child on self-performed exercises in a gradual mode.
Self-stretching: The joint stiffness and muscular weakness, which have occurred during immobilization are major problems so the self-stretching-hold technique to improve the ROM of the postimmobilization joint stiffness.
Orthoses: Provide proper orthoses if needed
Progression to exercises: Progress the exercise mode to antigravity or self-resistive one.
Functional activities: Guide the mother adequately to help the child to properly carry out functional activities as independently as possible and be alert
Friction massage: Prevention of formation of an adherent scar.
Besides ambulation, focus on achieving strong and maximum ROM at the hip and knee towards functional ambulation, with the limit of the process of recovery of the disease.
Complications
- Acute-on-chronic osteomyelitis: Acute exacerbations of a chronic disease can occur repeatedly and are treated with antibiotics, and drainage of pus, if required.
- Stiffness of the adjacent joints: This can occur due to the following: (a) Soft tissue contractures (b) Secondary septic arthritis
- Pathological fracture: This can occur through the weakened part of the bone. This is generally treated by conservative methods. However, nowadays, it can very well be treated by the Ilizarov fixation technique. 4. Deformity can occur due to the following: (a) Malunion of a pathological fracture (b) Premature arrest of the epiphyseal growth plate due to infection
- Limb length discrepancy (a) Shortening occurs when the growth plate is damaged due to infection. (b) Lengthening may occur occasionally because of increased vascularity in the region of the growth plate as a result of osteomyelitis.
- Malignancy: A long-standing discharging sinus may in rare cases transform into squamous cell carcinoma. Septic arthritis of the right hip joint.
Recent Post
8 best pain killers for muscle pain
8 best pain killers for muscle pain Pain is one of the most common health complaints worldwide, and pain killers are often the first solution
Immediate Gout Pain Relief Fast in 24 hours
Immediate Gout Pain Relief Fast in 24 hours Gout is a form of inflammatory arthritis caused by elevated serum uric acid levels, leading to the
5 Effective knee pain exercises at home
5 Effective knee pain exercises at home Knee pain exercises at home are a simple way to reduce pain, ease stiffness in an aching knee,

Why My Knee Hurt and Fix It?
Why My Knee Hurt and Fix It? Knee hurt is a common problem that can affect your daily routine, especially when walking, running, or climbing
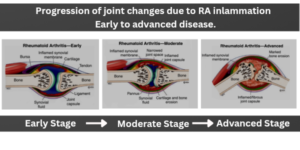
Understanding ALL about Rheumatoid arthritis
Rheumatoid arthritis Rheumatoid arthritis (RA) is a disease of synovium (a thin, soft connective tissue membrane that lines the inner surface of synovial joints) characteristics

Different menstrual cycle phases
Stages of menstrual cycle Phases Let’s start this article with my story of mensturation , I was 15 when I got my first period and
