Myasthenia gravis
Table of Contents
What is myasthenia gravis?
Myasthenia term means ” muscular weakness ” and gravis implies serious.
Myasthenia gravis is an organ-specific autoimmune disease. ) caused by antibodies to acetylcholine receptors in the post-junctional membrane of the neuromuscular junction. Which result in blockage of neuromuscular transmission and complement-mediated inflammatory response reduces the number of acetylcholine receptors and damages the end plate. It leads to fatigable
weakness and affects the ocular, facial, and bulbar muscles.
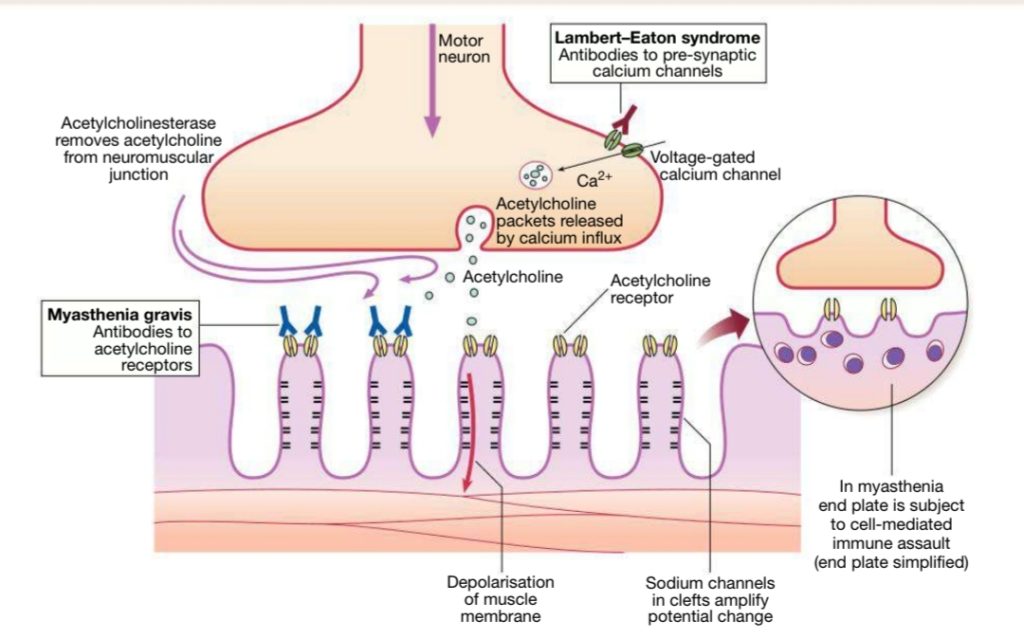
Myasthenia gravis usually presents between the ages of 15 and 50 years and there is a female preponderance in younger patients. In older patient, males are more commonly affected. It tends to run a relapsing and remitting course.
What are the signs & Symptoms of Myasthenia gravis?
- Weakness of the oculomotor muscles leads to central eye movement disorder.
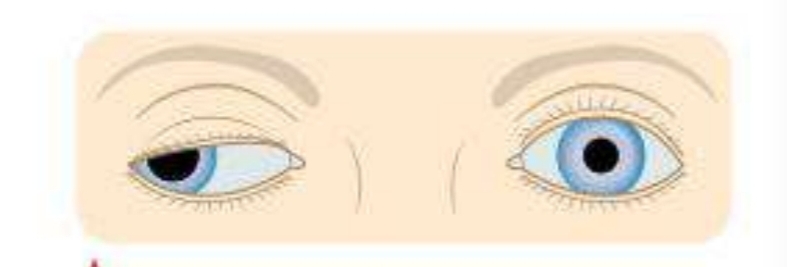
- Ptosis or diplopia
- Weakness of chewing, swallowing, speaking, or limb movement.
- Resting of the eyelids (looking downwards)
- Cogan’s lid twitch sign( increased reflex elevation with up-gaze )
- Any limb muscle may be affected, most commonly those of the shoulder girdle Example: the patient is unable to undertake tasks above shoulder level, such as combing the hair, without frequent rests.
- Respiratory muscles may be involved and respiratory failure is an avoidable cause of death.l. Ventilatory support is required where weakness is severe or of abrupt onset
How to diagnose Myasthenia gravis?
- Tensilon test: Intravenous injection of the short-acting anticholinesterase
edrophonium bromide. - Nerve conduction studies: Repetitive stimulation during nerve conduction studies may
show a characteristic decremental response. Serum testing: It is done for Anti-Acetylcholine Receptor Antibodies(AChR-Ab) present in blood .
- Enzyme-linked immunosorbent assay (ELISA)
The Ice-Pack Test: This safe and straightforward bedside investigation. It also provides symptomatic relief from ptosis .
Repetitive Nerve Stimulation: Muscle response to these stimulations and these patterns are studied for identification of Myasthenia gravis.
Treatment method for Myasthenia gravis ?
Acute treatments
Intravenous immunoglobulin
• Lowers production of antibodies and rapidly reduces weakness
Plasma exchange
• Removing antibody from the blood may produce marked improvement; this is usually brief, so is normally reserved for myasthenic crisis or for pre-operative preparation.
Long-term treatments
Glucocorticoid treatment
• Improvement is commonly preceded by marked exacerbation of myasthenic symptoms, so treatment should be initiated in hospital
• Usually necessary to continue treatment for months or years, risking adverse effects
Pharmacological immunosuppression treatment
• Azathioprine 2.5 mg/kg daily reduces the necessary dosage of glucocorticoids and may allow their withdrawal. Effect on clinical features may be delayed for months.
• Mycophenolate mofetil: less commonly used.
Thymectomy
• Should be considered in any antibody-positive patients under 45 years with symptoms not confined to extraocular muscles, unless disease has been established for more than 7 years.
• Likely to be required for thymoma.
Recent Post
Best 25 Heart Healthy Foods to Eat
Best 25 Heart Healthy Foods to Eat Heart disease remains one of the leading health concerns worldwide, but many risk factors can be managed through
Sharp Pain in the Heel of My Foot: Causes and Treatment
Sharp Pain in the Heel of My Foot: Causes and Treatment Pain in the heel of my foot is one of the most common foot
Why my heel hurts when i walk : Possible Reasons and Fixes
Why my heel hurts when i walk : Possible Reasons and Fixes Heel pain can make everyday activities difficult. Many people notice discomfort while getting

8 best pain killers for muscle pain
8 best pain killers for muscle pain Pain is one of the most common health complaints worldwide, and pain killers are often the first solution
Immediate Gout Pain Relief Fast in 24 hours
Immediate Gout Pain Relief Fast in 24 hours Gout is a form of inflammatory arthritis caused by elevated serum uric acid levels, leading to the
5 Effective knee pain exercises at home
5 Effective knee pain exercises at home Knee pain exercises at home are a simple way to reduce pain, ease stiffness in an aching knee,
